If you've been searching for answers about women's hair loss, you've probably encountered a wall of products, promises, and conflicting information. So let's cut through it.
Not all hair loss treatments are created equal — and for women especially, the options that work, why they work, and how to use them correctly are still widely misunderstood. What follows is a straightforward look at three treatments with real clinical evidence behind them: what the science says, what the experience is actually like, and where each one fits in your strategy.
The short version? They each have a role to play. And the third one might be the most overlooked — and most promising — of all.
#1: Minoxidil — The Proven Starting Point

What it is: A topical (or oral) medication applied directly to the scalp, available over the counter in 2% and 5% formulations. Minoxidil is the only FDA-approved medication specifically indicated for female-pattern hair loss.
How it works: Minoxidil widens blood vessels around hair follicles, improving circulation and nutrient delivery. It also appears to extend the anagen (growth) phase of the hair cycle and help follicles in the resting phase re-enter active growth. The result, with consistent use, is thicker, denser hair over time.
What the evidence shows: In clinical trials supporting FDA approval, 2% minoxidil produced moderate hair regrowth in 19% of women and minimal regrowth in 40% after 8 months — compared to 7% in the placebo group. The 5% formulation has shown even stronger results, with greater patient-perceived benefit and higher density improvements, though it comes with a slightly elevated risk of scalp irritation and unwanted facial hair in some users.
The honest tradeoffs: Minoxidil requires twice-daily application and long-term commitment — hair gains are typically lost within months of stopping. Roughly 40% of women don't respond meaningfully to it. It can also cause scalp irritation and, in some cases, an initial shedding phase that's alarming but temporary. Oral minoxidil (prescribed off-label at low doses for women) is an option for those who don't respond to topical use, but requires physician supervision due to potential systemic effects.
Best for: Women in the early-to-moderate stages of hair loss who want an established, well-studied first-line treatment and are prepared for the daily routine it requires.
#2: Spironolactone — The Hormonal Option
What it is: An oral prescription medication originally developed as a blood pressure drug, now widely prescribed off-label by dermatologists and gynecologists to treat hormonally-driven hair loss in women.
How it works: Spironolactone is an anti-androgen — it blocks the effects of DHT (dihydrotestosterone) and other androgens at the follicle level. Since androgens are often the primary driver of female-pattern hair loss (and a central issue in conditions like PCOS), targeting them directly can address the root cause rather than just the symptom.

What the evidence shows: A systematic review and meta-analysis found that oral spironolactone produces meaningful improvements in female-pattern hair loss, with the strongest results in women who have confirmed hormonal contributors — elevated androgens, PCOS, or hair loss that worsened during or after hormonal transitions like menopause or stopping hormonal birth control. It's particularly well-regarded by physicians who specialize in women's hormonal health.
The honest tradeoffs: Spironolactone is a prescription drug with real side effect considerations, including dizziness, elevated potassium, and menstrual irregularities. It is contraindicated in pregnancy, so women of childbearing age typically need to use contraception while taking it. It also addresses androgenic hair loss specifically — if your hair loss has non-hormonal roots (nutritional deficiency, thyroid dysfunction, stress-related shedding), it may not be the right tool.
Best for: Women whose hair loss is clearly linked to androgen excess — including those with PCOS, post-menopausal thinning, or hair loss that intensified after hormonal changes. Always requires a physician's evaluation and prescription.

#3: Low-Level Laser Therapy (LLLT) — The Underrated Game-Changer
This is where things get genuinely exciting.
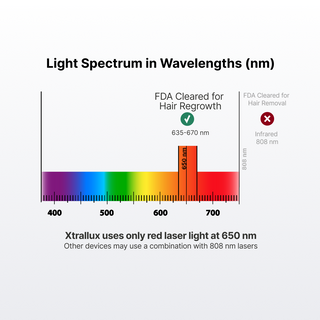
What it is: Low-level laser therapy (LLLT) — also called photobiomodulation — uses specific wavelengths of red or near-infrared light (typically 630–670 nanometers) to stimulate hair follicles at the cellular level. At-home devices, like the laser caps made by Xtrallux, bring this technology out of the clinic and into your daily routine.
How it works: When laser light at the right wavelength reaches the scalp, it's absorbed by mitochondria — the energy engines inside cells. This triggers a cascade of cellular activity: improved metabolism, increased blood flow to follicles, reduced inflammation, and a shift of follicles from the resting phase (telogen) back into active growth (anagen). It doesn't just temporarily change the hair you can see. It works at the level of the follicle itself.
What the evidence shows: The FDA cleared LLLT devices for hair regrowth — for both men and women — based on clinical trial data showing meaningful improvements in hair density, thickness, and shaft diameter. A randomized controlled trial in women with female-pattern hair loss found that LLLT combined with 2% minoxidil produced better hair diameter improvements than minoxidil alone. A separate study using LLLT plus 5% minoxidil found statistically significant gains in hair recovery at 6, 9, and 12 months compared to minoxidil monotherapy. Multiple peer-reviewed reviews consistently describe LLLT as well-tolerated, with no significant adverse effects — a stark contrast to medication-based approaches.
Crucially: LLLT has been studied specifically in women with female-pattern hair loss, not just extrapolated from male data. That matters.
Why Xtrallux stands out: Not all LLLT devices are equivalent, and the differences are meaningful. Xtrallux laser caps use clinical-grade laser diodes — not LEDs, which scatter light and lack the penetrating precision of true laser energy. The cap design delivers consistent, full-scalp coverage in every session. Devices are FDA-cleared. And the protocol — 30 minutes, every other day — is designed to fit into real life. You wear the cap, go about your morning, and take it off. No residue, no prescription, no recovery time.
For women who have tried minoxidil and found it inconvenient, ineffective, or irritating — or who want to treat hair loss without any systemic medication — LLLT offers something genuinely different: a drug-free, non-invasive, clinically supported option that works with your biology rather than overriding it.
The honest tradeoffs: LLLT is not a quick fix. Consistent, every-other-day use over three to six months is where results emerge. The investment is front-loaded (the device itself), rather than ongoing (monthly product purchases), which many women find preferable in the long run. And because LLLT works at the follicle level rather than through systemic pathways, it pairs naturally with other treatments rather than competing with them.
Best for: Women at any stage of hair loss who want a drug-free, non-invasive, clinically validated option — especially those who haven't responded fully to minoxidil, have hormonal contributors being managed separately, or simply want to address hair loss without adding another medication to their routine.
How These Treatments Work Together
The good news: these three approaches aren't mutually exclusive. In fact, the most effective strategies often combine them.
Minoxidil addresses follicle dormancy and circulation. Spironolactone targets the androgenic root cause. LLLT works at the cellular level to revitalize follicles from within and enhance the effects of other treatments. Clinical evidence supports combining LLLT with minoxidil for better outcomes than either alone — and for women managing hormonal hair loss, addressing androgen excess while supporting follicular health simultaneously is a smart, integrative strategy.
Think of it this way: if you're treating the cause with spironolactone, stimulating the surface with minoxidil, and energizing follicles with LLLT — you're approaching the problem from every angle that matters.
The Bottom Line
Female hair loss is real, it's common, and it's treatable. The three options above have genuine clinical evidence behind them — not marketing claims, not anecdote. Each has a place, each has tradeoffs, and the right combination depends on your specific situation, your hormonal profile, and your preferences around medication.
What we know with confidence: the earlier you act, the more options you have. Hair follicles that are dormant can often be reawakened. Follicles that have completely disappeared cannot. Which means the best time to start is now — with the treatments most likely to work for you.
Frequently Asked Questions
What is the most effective hair loss treatment for women? The most effective approach for most women combines treatments that address different mechanisms. Topical minoxidil is the only FDA-approved medication for female-pattern hair loss and remains a strong first-line option. For women with hormonal contributors, spironolactone targets androgen-driven thinning at the source. Low-level laser therapy (LLLT) is FDA-cleared, drug-free, and has clinical evidence supporting its use in women — particularly as a complement to minoxidil for improved outcomes.
Is LLLT proven to work for women's hair loss? Yes. Multiple randomized controlled trials have demonstrated LLLT's effectiveness in female-pattern hair loss specifically. Clinical evidence shows improvements in hair density, shaft diameter, and hair count with consistent use. The FDA has cleared LLLT devices for hair regrowth in both men and women. Studies combining LLLT with minoxidil have shown better results than either treatment alone.
What is the difference between Xtrallux and other LLLT devices? Xtrallux laser caps use clinical-grade laser diodes rather than LEDs. This distinction is significant: laser light is coherent and penetrates to the depth of the hair follicle, while LED light scatters and cannot replicate that precision. Xtrallux devices are FDA-cleared, designed for full-scalp coverage, and built for a realistic every-other-day protocol.
Can I use LLLT with minoxidil at the same time? Yes — and research suggests the combination may outperform either treatment alone. LLLT and minoxidil work through different mechanisms, making them complementary. A randomized controlled trial found that LLLT combined with minoxidil produced statistically significant gains in hair recovery at 6, 9, and 12 months that minoxidil monotherapy did not achieve.
How long does it take for LLLT to work? Most women using LLLT devices notice a reduction in shedding within the first few weeks of consistent use. Visible improvements in density and thickness typically emerge between three and six months. Results follow the natural rhythm of the hair growth cycle, so consistency — every other day, without long gaps — is the most important variable.
Is spironolactone safe for women with hair loss? Spironolactone is widely prescribed off-label for women's hair loss, particularly when there are hormonal contributors like PCOS or elevated androgens. It has a well-established safety profile in women, but it requires a physician's evaluation and prescription, is contraindicated in pregnancy, and may cause side effects including dizziness and menstrual changes. It is not appropriate for all women with hair loss — a dermatologist or hormone specialist can help determine if it's right for you.
At what stage of hair loss should I start treatment? As early as possible. Hair follicles that are miniaturized or dormant can often be stimulated back into growth. Follicles that have been lost completely cannot. Early intervention — before thinning becomes severe — gives every treatment a better chance of producing meaningful results.
References
- Olsen EA, Dunlap FE, Funicella T, et al. A randomized clinical trial of 5% topical minoxidil versus 2% topical minoxidil and placebo in the treatment of androgenetic alopecia in men. Journal of the American Academy of Dermatology. 2002;47(3):377–385. https://doi.org/10.1067/mjd.2002.124088
- Kenvue Brands LLC. Women's Rogaine Unscented — minoxidil foam [package insert]. Updated November 2024. DailyMed. https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=4d328537-b7f5-43cc-9837-c5a0c6c390f8
- Penha MA, Miot HA, Kasprzak M, Müller Ramos P. Oral minoxidil vs topical minoxidil for male androgenetic alopecia: a randomized clinical trial. JAMA Dermatology. 2024;160(6):600–605. https://doi.org/10.1001/jamadermatol.2024.0284
- Rathnayake D, Sinclair R. Use of spironolactone in dermatology. Skinmed. 2010;8(6):328–332.
- Aleissa M. The efficacy and safety of oral spironolactone in the treatment of female pattern hair loss: a systematic review and meta-analysis. Cureus. 2023;15(8):e43559. https://doi.org/10.7759/cureus.43559
- Avci P, Gupta GK, Clark J, Wikonkal N, Hamblin MR. Low-level laser (light) therapy (LLLT) for treatment of hair loss. Lasers in Surgery and Medicine. 2014;46(2):144–151. https://doi.org/10.1002/lsm.22170
- Zarei M, Wikramanayake TC, Falto-Aizpurua L, Schachner LA, Jimenez JJ. Low-level laser therapy and hair regrowth: an evidence-based review. Lasers in Medical Science. 2016;31(2):363–368. https://doi.org/10.1007/s10103-015-1818-2
- Pillai JK, Mysore V. Role of low-level light therapy (LLLT) in androgenetic alopecia. Journal of Cutaneous and Aesthetic Surgery. 2021;14(4):385–391. https://doi.org/10.4103/JCAS.JCAS_218_20
- Xiao C, et al. Comparative efficacy of 2% minoxidil alone against combination of 2% minoxidil and low-level laser therapy in female pattern hair loss — a randomized controlled trial in Chinese females. Journal of Cosmetic Dermatology. 2024. https://doi.org/10.1016/j.jcosder.2024.01.005
- Faghihi G, et al. Effectiveness of low-level laser therapy combined with topical minoxidil 5% solution in the treatment of androgenic alopecia. Journal of Research in Medical Sciences. 2013;18(8):647–650.
- Jean-Pierre P, Pulumati A, et al. Lasers in the management of alopecia: a review of established therapies and advances in treatment. Lasers in Medical Science. 2024;39(1):102. https://doi.org/10.1007/s10103-024-04054-7. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11023987/
- Rodrigues BL, et al. Female-pattern hair loss: therapeutic update. Anais Brasileiros de Dermatologia. 2023;98(4). https://pmc.ncbi.nlm.nih.gov/articles/PMC10334345/
- Kim H, et al. Low-level light therapy and minoxidil combination treatment in androgenetic alopecia: a review of the literature. Photobiomodulation, Photomedicine, and Laser Surgery. 2023. https://pmc.ncbi.nlm.nih.gov/articles/PMC10015651/
- Alosaimi A, Algarni A, Alharbi A, et al. Comparative efficacy of minoxidil alone versus minoxidil combined with low-level laser therapy in the treatment of androgenic alopecia: a systematic review and meta-analysis. Journal of Dermatological Treatment. 2025;36(1):2447355. https://doi.org/10.1080/09546634.2024.2447355
- Abdallah M, et al. Consensus recommendations for the management of androgenetic alopecia in Egypt: a modified Delphi study. PMC. 2025. https://pmc.ncbi.nlm.nih.gov/articles/PMC12533493/
This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare provider before beginning any hair loss treatment.